THE BRAIN
THE MENINGES
The body goes to great lengths to feed and protect the central nervous system. Part of the protective mechanism is found in the meninges which are membranes that envelop the central nervous system. The meninges consist of three layers: the dura mater, the arachnoid mater (membrane), and the pia mater.
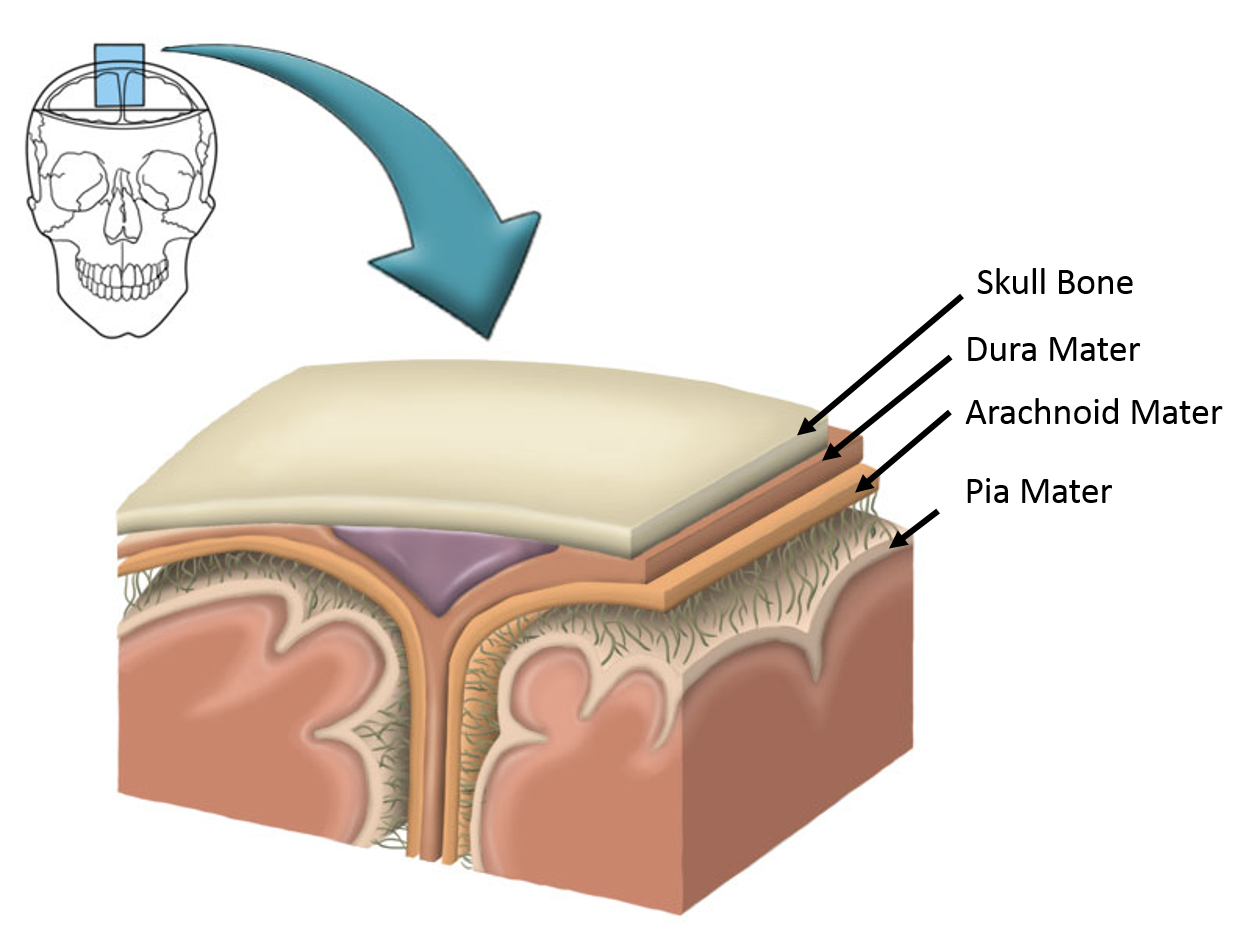
Image was drawn by a BYU-Idaho student Winter 2014.
The dura mater is a thick, tough, and durable membrane composed of dense fibrous connective tissue. The dura mater of the brain is composed of two layers, an outer periosteal layer that connects to the inside of the skull, and a deep meningeal layer. In certain areas these two layers separate and the meningeal layer forms folds that extend into the brain forming physical partitions in the brain. The Falx cerebri separates the two cerebral hemispheres, the tentorium cerebelli separates the occipital lobes of the cerebrum from the cerebellum; and the falx cerebelli separates the two cerebellar hemispheres.
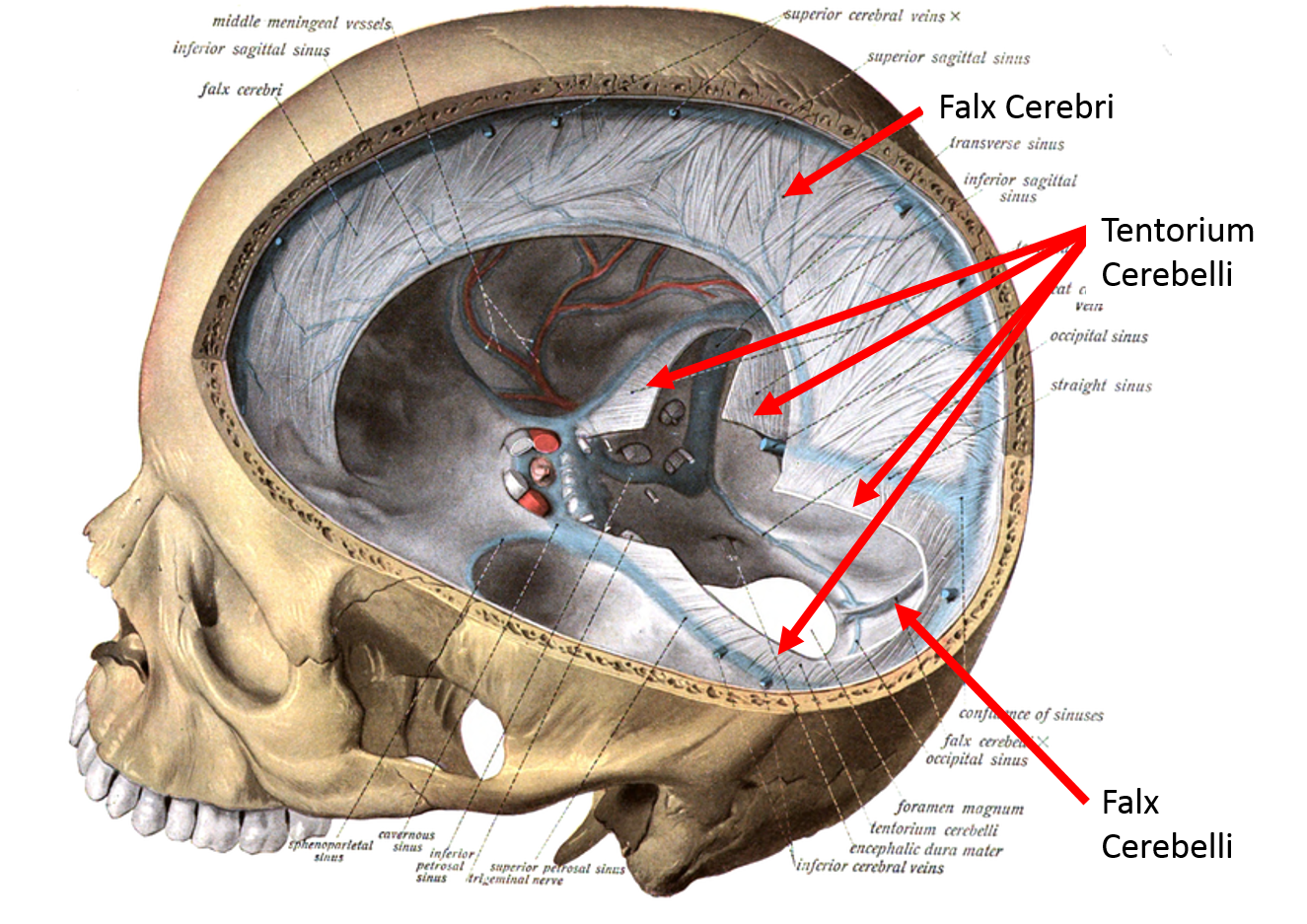
From Sobotta's Human Anatomy 1908. Public Domain.
The arachnoid mater or arachnoid membrane is directly under the dura mater. These two membranes are not physically connected and there is a space (more like a virtual space) between the dura mater and the arachnoid mater. The arachnoid mater is a very thin and transparent membrane that lies on top of a fluid filled space directly inferior to the membrane. This space, the subarachnoid space, is filled with cerebropinal fluid. The arachnoid membrane together with the cerebral spinal fluid helps to cushion the central nervous system and fits like a loose sac over it.
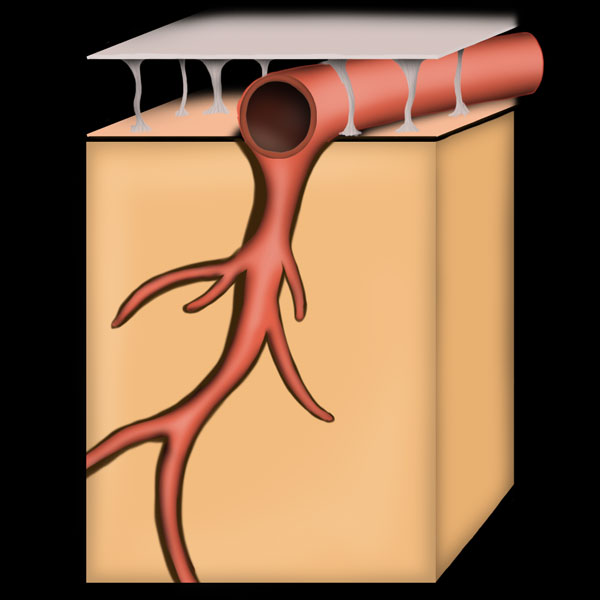
Image drawn by BYU-Idaho Student Spring 2014.
The arachnoid mater got its name from the many processes that extend down from the membrane through the subarachnoid space to the pia mater on the brain surface. These processes are very fine and look a bit like spider web fibers.
The pia mater is a very delicate membrane that adheres to the surface of the brain and spinal cord, following the contours (gyri and sulci) of the brain. The cerebral spinal fluid of the central nervous system sits on top of the pia mater (and underneath the arachnoid membrane).
There are some subtle differences between the meninges of the brain and the spinal cord, primarily with the dura mater. First, the dura mater of the spinal cord is composed of just a single layer, rather than two like we described in the brain. Second, the dura mater does not connect to the bones of the vertebra, instead, there is a space between the vertebra and the dura mater called the epidural space. This space is filled with a adipose that acts as a cushion and helps protect the spinal cord.
CERBROSPINAL FLUID
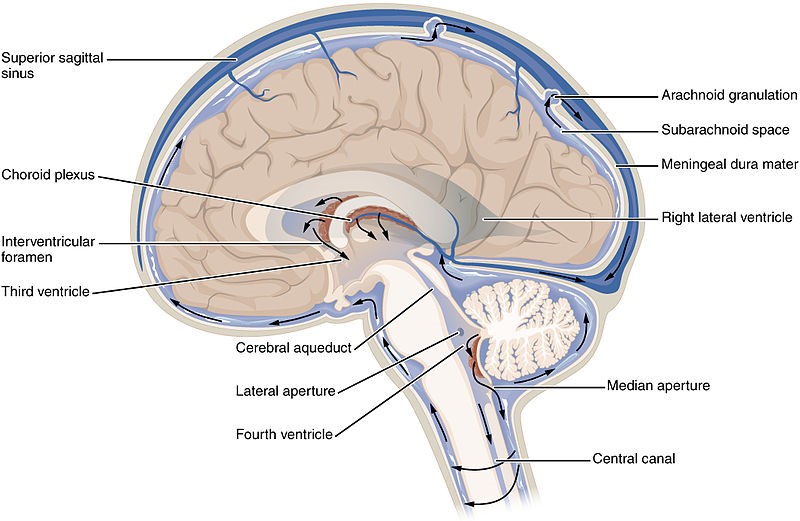
Cerebrospinal fluid (CSF) is the “blood” of the brain and spinal cord. It is produced in a structure called the choroid plexuses by ependymal cells.
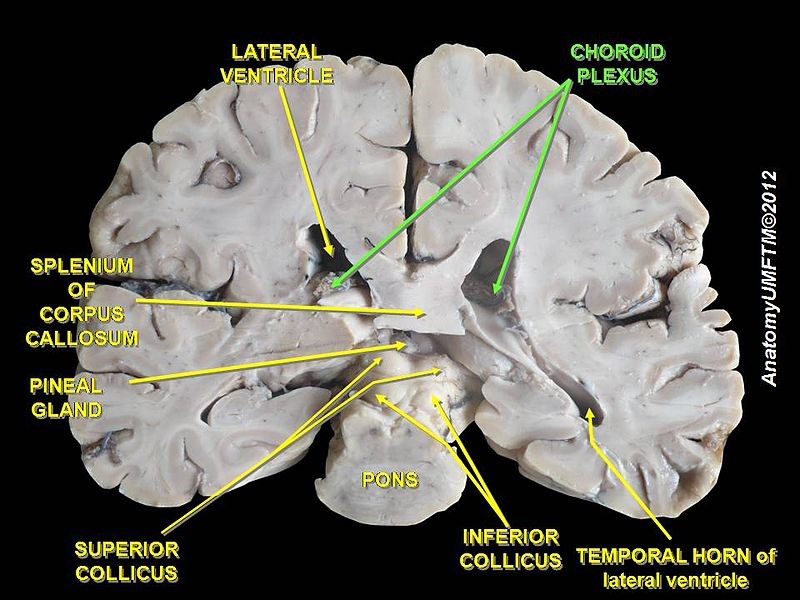
Author: Anatomist90; Wikimedia commons download Spring 2014; License: Creative Commons Attribution-Share Alike 3.0
These structure our found lining the ventricles of the brain. The majority of CSF is produced within the two lateral ventricles. The CSF is found in the subarachnoid space or the space between the arachnoid mater and the pia mater. The total amount of CSF in the brain ranges from 100-600ml, but it is produce and reabsorbed at a rate of 500ml per day. Ependymal cells produced CSF from the blood plasma making the contents of the CSF almost identical to the blood plasma, with the exception of proteins. The function of the CSF can be summarized into five categories:
1. Buoyancy: The CSF helps to suspend the brain which reduces the effective weight by 95%. This allows the brain to exist in a state called neutral buoyancy. In less scientific terms, it allows the weight of the brain to not squish itself.
2. Electrolyte and circulatory balance: The CSF is very important in maintaining the homeostatic balance of electrolytes and glucose.
3. Protection: The properties of water allow the CSF to serve as a protection against jolts.
4. Circulation: Although the CSF is a very low pressure system, it is an effective method of moving nutrients and waste around. It also helps to facilitate blood perfusion.
5. Waste removal: The CSF has proven essential in flushing metabolic waste. Recently researchers have shown that the flushing of waste is increased during sleep.
Sometimes a breach can occur, such as physical trauma or a lumbar puncture resulting in leakage of the CSF. This can change the pressure and allow the brain to not be as buoyant, which squishes on nerves and causes a variety of symptoms. In addition, in other cases a condition called hydrocephalus can occur. Hydrocephalus is the accumulation of CSF because of impaired flow or excessive production of CSF. This can also result in pressure changes and if it occurs in the fetus it can result in an enlarged head. Hydrocephalus in an adult must be immediately corrected.
TRAUMATIC BRAIN INJURY
There are different types of hemorrhages that can occur in the central nervous system. We will discuss the four major types: epidural, subdural, subarachnoid and intracerebral hemorrhages.
Epidural hemorrhages occur between the dura mater and the skull and are usually very rapid because the hemorrhage comes from damage to the arteries along the inside of the skull. Recall looking at the skulls in lab and seeing the grooves where the arteries of the skull once ran. These arteries are under high pressure vessels bleed rapidly when damaged. This bleeding results in a hematoma, which strips the dura membrane off the skull as it expands, causing intense headaches. More seriously is the compression of the nervous system as the hematoma expands against the skull. The most common cause of epidural bleeds is a skull fracture which lacerates these arteries. Epidural hemorrhages can be fatal if left untreated. Treatment is done by surgically draining or removing the hematoma to relieve pressure on the brain.
Subdural hemorrhages occur between the dura mater and the brain. These result from tears in the veins that cross the subdural space in response to a head injury, especially rotational or linear forces. Subdural hemorrhages are classic injuries found in shaken baby syndrome and severe whiplash. They are also more common in people on aspirin, since aspirin inhibits blood clotting. They can be subdivided into acute, subacute and chronic subdural hematomas depending on the severity of the hemorrhage. Acute hematomas develop rapidly and are the most severe with a mortality rate of 60 to 80%. Subacute hematomas fall into the same category although slightly less severe. Chronic subdural hematomas develop over a period of days to weeks and often result from minor head trauma (like a concussion). Symptoms of subdual hemorrhage typically have a slower onset than epidural bleeds because the bleeding comes from veins instead of arteries.
Author: OpenStax College; Downloaded Spring 2014.
License: Creative Commons Attribution 3.0 Unported license.
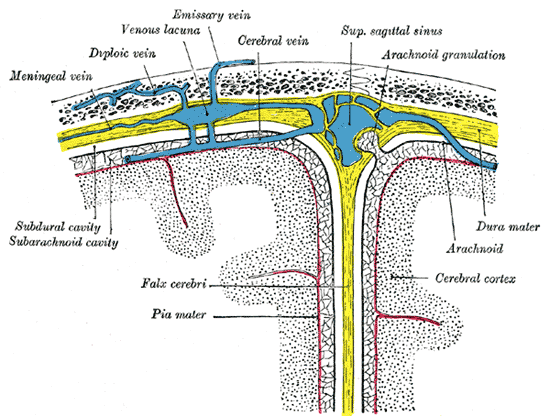
Grays Anatomy: Public Domain
To understand subdural hemorrhages better, it helps to examine the anatomy. Notice that veins from the brain cross the subarachnoid space and pierce both the arachnoid and dura mater to finally dump venous blood in the superior sagittal sinus. When whiplash, shaking or any type of rapid, intense linear motion occurs, the brain moves inside the skull. Very much movement will put tension on the veins where they pierce the arachnoid and dura mater membranes. The arachnoid membrane moves relatively easy compared to the dura mater. A shearing effect can occur where the vein is broken off just superior to the arachnoid membrane. Blood slowly starts to fill the space between the arachnoid and dura maters.
Subarachnoid hemorrhages occur in the area between the arachnoid membrane and the pia mater that surrounds the brain (remember this is where the cerebral spinal fluid is found). There are many arteries in the subarachnoid space as it is this space that blood vessels like the internal carotid arteries enter. The bleeding may occur by spontaneous rupture or as a result of head injury. The most common symptom is called the thunderclap headache, or one that develops immediately within seconds and feels like a kick in the head.
Intracerebral hemorrhages occur within the brain tissue itself and usually involve very small blood vessels. This type of hemorrhage may be caused by trauma or spontaneous rupture. Symptoms are associated with the functional area of the brain that is experiencing the trauma. Intracerebral hemorrhages are the second most common cause of stroke and the risk of experiencing this type of hemorrhage is increased by high blood pressure and diabetes.
**You may use the buttons below to go to the next or previous reading in this Module**


